Can Thyroid Disorders Cause Allergies?
Allergies are defined as a hypersensitive immune response to a substance that either enters the body or touches the skin.
Millions of people in the United States and across the globe have an allergic reaction to something and experience symptoms that vary from mild to severe.
The exact cause of allergies is unknown, but various factors can make our body react in that manner.
Could thyroid problems cause allergies?
Thyroid and allergies
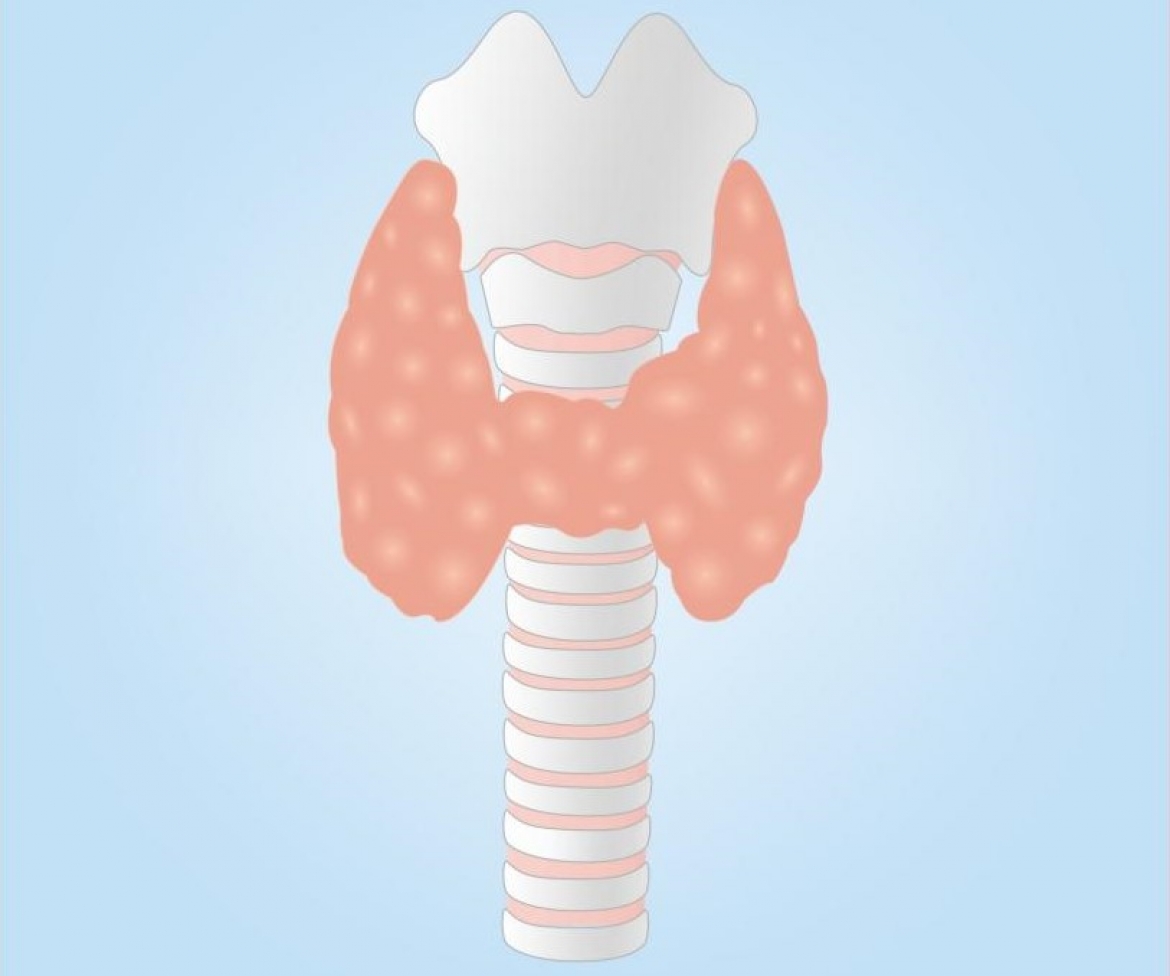
Conditions affecting the butterfly-shaped gland have a strong influence on the functions of other glands, tissues, and organs in our body.
Bearing in mind that thyroid diseases are associated with many other health concerns we experience, it is natural to wonder whether they could also cause allergies. The truth is that the relationship between allergies and thyroid function is complicated, and extensive research is needed to uncover all its mechanisms.
The subject is, at this point, insufficiently explored and it will be necessary to change that in the future.
Autoimmune thyroid diseases common in allergic rhinitis
Despite the wide prevalence of thyroid diseases, there is still a lot we need to learn about them. Autoimmune thyroid diseases, Hashimoto’s thyroiditis, and Graves' disease are the most common autoimmune conditions.
Allergic conditions are also common.
Is there a link between some of those conditions such as allergic rhinitis and autoimmune thyroid diseases? It turns out there could be an association between them.
Degirmenci et al. carried out a study whose primary objective was to analyze the incidence of autoimmune thyroid disease in patients with allergic rhinitis. Allergic rhinitis, also known as hay fever, is an allergic response to specific allergens such as pollen.
According to the American Academy of Allergy, Asthma, and Immunology, about 7.8% of adults in the US have some kind of hay fever. On a global level between 10% and 30% of the world population is affected by allergic rhinitis[i].
So, let’s get back to the above-mentioned study. Scientists enrolled 1239 patients with allergic rhinitis and 700 healthy subjects.
For the purpose of the research, their thyroid hormone levels were measured. Results showed that 171(13.8%) participants with allergic rhinitis had euthyroid Hashimoto's thyroiditis and 31 (2.5%) had hypothyroid Hashimoto's thyroiditis.
On the other hand, 688 (98.2%) healthy participants had normal thyroid function, 10 (1.4%) had euthyroid Hashimoto's thyroiditis, and two (0.4%) had hypothyroid Hashimoto's thyroiditis.
Scientists concluded that the incidence of Hashimoto's thyroiditis was greater in subjects with allergic rhinitis compared to their healthy counterparts[ii]. Therefore, these findings confirm that there is a link between allergies and thyroid conditions.
Allergy in autoimmune thyroid diseases
As mentioned above, Hashimoto’s thyroiditis is more common among people with allergic rhinitis than in the general population.
That means people with allergies, at least some of them, are more prone to autoimmune thyroid diseases. But does vice versa also apply?
Molnar et al. conducted a study to evaluate the relationship between allergy and autoimmune thyroid diseases i.e., whether people with these conditions are more prone to allergies. For that purpose, they enrolled 259 patients, of whom 149 had Graves' disease, 110 had Hashimoto's thyroiditis, and 65 controls with small euthyroid goiter.
They analyzed participants' thyroid hormone levels and allergen-specific IgE levels. Immunoglobulin type E (IgE) is a type of antibody that plays a central role in acute allergic reactions and chronic inflammatory allergic diseases. Their findings revealed that the prevalence of respiratory and food allergen-specific IgE levels were higher in subjects with Graves' disease compared to people with Hashimoto's thyroiditis and healthy controls.
Moreover, the study also showed that the seasonal allergen-specific IgE levels increased more in Graves' disease patients without ophthalmopathy (disorder affecting orbit and periorbital tissues of the eyes) than in subjects who had this eye disease. Scientists also found that the presence of allergen-specific IgE levels was linked to changes in thyroid hormone and anti-thyroid antibody levels.
In other words, the study showed that patients with autoimmune thyroid conditions (particularly Graves' disease) had increased levels of allergens in their body. This confirms the link between thyroid conditions and allergies.
Since allergies are associated with increased production of pro-inflammatory cytokines, they may also aggravate or even induce autoimmune thyroid diseases[iii].
Selvendran and Aggarwal wrote about a case study of a hypothyroid woman who also developed chronic urticaria, an allergic condition of the skin. The patient received thyroxine to treat her hypothyroidism.
Four weeks later, her chronic urticaria symptoms resolved too. Scientists reported that 5% to 34% with chronic urticaria have anti-thyroid antibodies, and 5% to 10% have clinically or biochemically apparent thyroid disease.
The relationship between thyroid disease and allergy was evident here, but the underlying cause remained unknown. Researchers pointed out that the link between thyroid disease and allergy is mysterious. Some factors could include elevated IgG anti-thyroid autoantibodies, increased production of pro-inflammatory cytokines[iv].
A different study, carried out by Goncalves Missaka et al., found that chronic idiopathic urticaria and autoimmune thyroid disease presented a greater risk of angioedema (swelling of deeper skin layers). These findings reinforce the idea that a relationship exists between thyroid problems and allergy[v].
It doesn’t mean you’ll have allergy for sure
The fact that various studies confirmed the link between allergy and thyroid it doesn’t really mean you’ll have allergic condition or reaction to something just because you have hypothyroidism or some other thyroid-related disease.
The relationship between thyroid problems and allergies is complicated. Various mechanisms are involved in the process.
For example, if thyroid hormone levels are low, you may develop some symptoms that are similar to allergies such as hives, itching, eye discomfort, and nasal congestion. These symptoms do not necessarily mean you have an allergy.
Men and women who have some thyroid disease, a particular autoimmune condition, should see their doctor regularly. Proper management of their condition is crucial for keeping allergy symptoms at bay too.
Plus, if you develop some allergy condition, your doctor would be able to spot it if you see them regularly.
Why we get allergies?
Throughout this article, we have talked about allergies in relation to the thyroid condition, and it's important to address a thing or two about this common issue. While we all know what allergies are, most of us, don't know much beyond that.
The question most people want to know is how we get allergy in the first place.
As mentioned at the beginning of the article, the exact cause that induces allergy is unknown, and scientists are still trying to discover why immune system causes an allergic reaction when a harmless foreign substance enters the body. IgE causes the reaction, but it’s not quite known why the body releases those antibodies.
When a man or a woman with an allergy comes in contact with the allergen, the body doesn't react immediately. The immune system gradually builds up a sensitivity to the substance, and eventually, it overreacts.
That happens because the immune system needs some time to identify and remember that specific allergen. Over time, as it becomes sensitive to the allergen, the immune system starts producing antibodies whose mission is to attack and destroy it.
This process of antibodies production to attack allergens is called sensitization, and it takes a few days or several years. It's also possible for the sensitization process to remain incomplete. When that happens, a person experiences some symptoms but not a full allergy.
What we do know is that allergies have a genetic component. In other words, if your parents have some allergy condition, you are at a higher risk as well. But, it’s important to clarify one thing – only the risk to an allergic reaction is genetic. Children do not inherit specific allergens.
For instance, if your father is allergic to nuts, it doesn't mean you will have nut allergy as well.
The most common allergens include:
- Foods – nuts, milk, wheat, shellfish, egg
- Insect stings – bees, mosquitoes, wasps
- Animal products – pet dander, dust mite waste
- Plants – pollen, resin from poison ivy, etc.
- Drugs – penicillin etc.
- Mold – airborne spores
- Other allergens – latex, metals, etc.
Various factors can increase your risk of allergy including a family history of allergies and asthma, being a child, not being exposed to enough sunlight, having asthma, birth by Caesarian section, and already having some type of allergy.
Allergy FAQs
If I didn’t develop an allergy in childhood, it means I'm safe in adulthood?
Not really. We tend to associate allergies to childhood because we are more likely to develop them when we’re kids. However, the reality is that a person can become allergic to something at any age.
Allergies can affect anyone regardless of how old they are or their socioeconomic status. In other words, while children are more likely to have allergies, they can occur for the first time at any age. In some cases, allergies can recur after many years of remission.
Is there a cure for allergies?
It would be ideal if we would be able to take a pill or get a shot and eliminate allergy forever. Unfortunately, that’s not how it works. We can’t cure or eliminate allergy entirely, but we can manage symptoms and reduce their severity.
After allergy diagnosis, the doctor recommends adequate treatment measure and proposes some lifestyle adjustments you should make. Management of allergies requires a little bit of work and effort, but it’s entirely achievable.
What drugs do doctors prescribe for allergies?
Good news is that most drugs for allergies are available in the over-the-counter form i.e., they do not require doctor's prescription. This doesn't mean you should skip the doctor. In fact, you shouldn't buy drugs for allergy just because you think you have it. It's more useful to see the doctor, undergo the test, and get a diagnosis.
Plus, the doctor can recommend the most adequate drugs for your specific case. The most common drugs for allergies include antihistamines, decongestants, steroid sprays, and leukotriene receptor antagonists or anti-leukotrienes.
What is immunotherapy?
Immunotherapy or hyposensitization is a treatment approach whose main goal is to rehabilitate the immune system to induce long-term tolerance.
The doctor administers increasing doses of allergens over a few-year period to reduce the production of IgE. This is only recommended to men and women with severe allergies when other treatment options don’t work.
Is my allergy linked to stress?
It could be. Bear in mind that stress doesn't cause allergy per se, but it can worsen existing allergic reaction through elevated levels of histamine in the blood. Histamine can cause symptoms of allergy.
That's why it's important to manage stress. It's also worth noting that stress and thyroid also have a strong two-way relationship. Find a way to rest and relax, instead of ignoring stress, make sure you resolve it. That way, you'll feel better and healthier.
Allergy in numbers
- About 10% of the world's population experiences adverse drug reactions
- 20% of hospitalized patients have an allergic reaction to some drug
- Survey of 38,480 children (ages 0 to 18) showed that 8% had a food allergy
- The increased prevalence of allergies in the industrialized world has continued for more than 50 years
- 32 million Americans have a food allergy
- 40% of children with food allergy are allergic to more than one food[vi]
Conclusion
Allergies are common problems whose prevalence has been growing continuously.
The relationship between thyroid problems and allergy is poorly studied, but current evidence shows they do influence one another.
People with thyroid problems should see their doctor if they experience allergy-like symptoms.
References
[i] Allergy statistics, Allergic rhinitis. American Academy of Allergy, Asthma, and Immunology. Retrieved from: https://www.aaaai.org/about-aaaai/newsroom/allergy-statistics
[ii] Degirmenci PB, Kirmaz C, Oz D, et al. (2015). Allergic rhinitis and its relationship with autoimmune thyroid diseases. American Journal of Rhinology and Allergy, 29(4):257-61. Doi: 10.2500/ajra.2015.29.4189. Retrieved from: https://www.ncbi.nlm.nih.gov/pubmed/26067918
[iii] Molnar I, Kelemen E, Somogyine-Vari E. (2015). The prevalence and characteristics of allergy in autoimmune thyroid diseases. Journal of Clinical and Cellular Immunology, 6:306. Doi: 10.4172/2155-9899.1000306. Retrieved from: https://www.omicsonline.org/open-access/the-prevalence-and-characteristics-of-allergy-in-autoimmune-thyroid-diseases-2155-9899-1000306.php?aid=51713
[iv] Selvendran, S. S., & Aggarwal, N. (2018). Chronic urticaria and thyroid autoimmunity: a perplexing association. Oxford medical case reports, 2018(2), omx099. doi:10.1093/omcr/omx099. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5822693/
[v] Gonclaves Missaka RFB, Costa Penatti H, Cavarini Silvares MR, et al. (2012). Sao Paolo Medical Journal, 130(5). Doi: 10.1590/S1516-31802012000500005. Retrieved from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1516-31802012000500005
[vi] Food allergy 101, facts, and statistics. Food Allergy Research and Education. Retrieved from: https://www.foodallergy.org/life-with-food-allergies/food-allergy-101/facts-and-statistics



















































Leave a comment